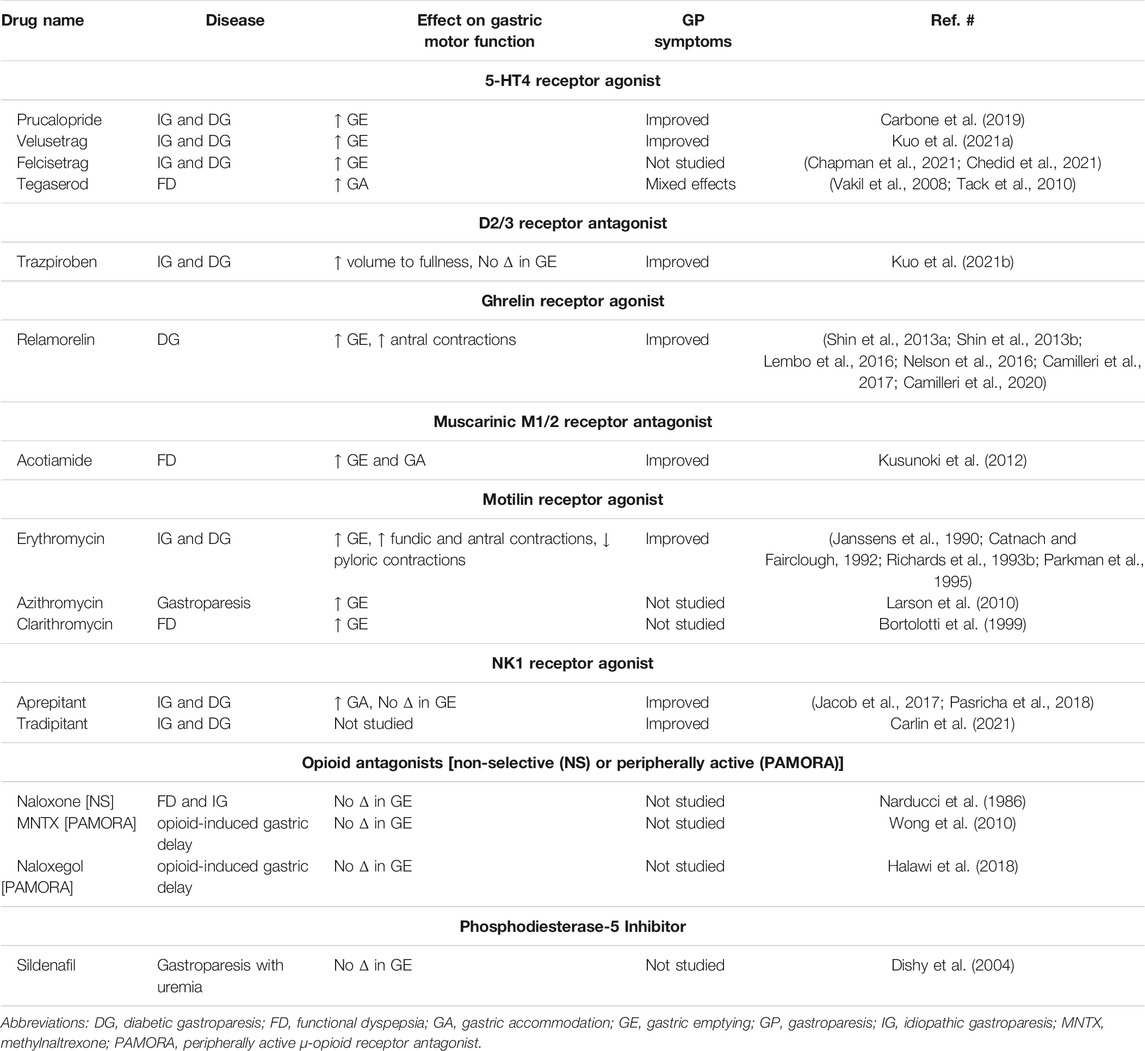
Azithromycin isn’t typically used to directly improve gastric motility. Its primary function is as an antibiotic. While some studies suggest potential indirect effects on gut motility, there’s no established azithromycin dosage specifically for this purpose.
Instead of relying on azithromycin, consider proven methods to enhance gastric motility. These include dietary changes, such as avoiding trigger foods, and lifestyle modifications like regular exercise. If symptoms persist, consult a gastroenterologist to explore options like prokinetics (e.g., metoclopramide) or other appropriate treatments.
Remember, self-medicating can be harmful. Always discuss any medication, including antibiotics like azithromycin, with your physician before use. They can accurately assess your condition and recommend a safe and effective treatment plan tailored to your needs. A thorough examination is crucial to determine the underlying cause of your gastric motility issues.
Disclaimer: This information is for educational purposes only and should not be considered medical advice. Always consult a healthcare professional for diagnosis and treatment.
- Azithromycin and Gastric Motility: A Concise Overview
- Clinical Implications
- Further Research
- Azithromycin’s Impact on Gastric Emptying Time
- Clinical Relevance of Azithromycin’s Effects on Gastric Motility
- Dosage Considerations and Patient-Specific Factors
- Renal and Hepatic Impairment
- Age and Weight
- Concomitant Medications
- Underlying Medical Conditions
- Monitoring Response
- Disclaimer:
- Future Research Directions and Unanswered Questions
Azithromycin and Gastric Motility: A Concise Overview
Azithromycin’s impact on gastric motility remains complex and not fully understood. While some studies suggest a potential for minor delays in gastric emptying, significant clinically relevant effects are rare. The drug primarily targets bacterial infections, not the gastrointestinal tract’s motor function.
Clinical Implications
Clinicians should consider individual patient factors. Patients with pre-existing motility disorders might experience heightened sensitivity. However, routine dosage adjustments for azithromycin based solely on anticipated effects on gastric motility aren’t typically warranted. Monitoring for potential gastrointestinal side effects, such as nausea or vomiting, is standard practice when prescribing azithromycin. These effects are often unrelated to direct motility changes and usually resolve spontaneously.
Further Research
More research is needed to fully elucidate azithromycin’s effects on gastric motility across diverse populations and disease states. This will help refine clinical guidelines and improve patient care.
Azithromycin’s Impact on Gastric Emptying Time
Azithromycin’s effect on gastric emptying time is complex and not fully understood. Studies show varying results, with some indicating a slight delay in gastric emptying, while others find no significant impact. This variability likely stems from factors including dosage, patient characteristics (age, comorbidities), and study methodology.
A meta-analysis of available research is needed to draw definitive conclusions. Currently, there’s insufficient evidence to definitively state whether a clinically significant delay occurs consistently. Clinicians should consider individual patient factors when prescribing azithromycin, particularly in patients with pre-existing gastrointestinal issues or those taking medications that affect gastric motility.
For patients experiencing delayed gastric emptying symptoms after azithromycin administration, alternative antibiotics should be considered, if possible, especially in cases requiring rapid drug absorption. Monitoring of symptoms and close clinical observation are recommended in all patients receiving azithromycin.
Further research focusing on standardized methodologies and larger patient populations is crucial to clarify azithromycin’s impact on gastric emptying time and to develop specific recommendations for clinical practice.
Clinical Relevance of Azithromycin’s Effects on Gastric Motility
Azithromycin’s impact on gastric motility is clinically significant, primarily due to its potential to delay gastric emptying. This effect varies depending on dosage and individual patient factors.
Specifically:
- Delayed gastric emptying can prolong the absorption of co-administered drugs, potentially altering their therapeutic effects or increasing the risk of adverse events.
- This delay is more pronounced with higher azithromycin doses.
- Patients with pre-existing gastrointestinal motility disorders are particularly vulnerable to experiencing exacerbated symptoms, such as nausea and vomiting.
Clinicians should consider these factors when prescribing azithromycin, especially when concomitant medications with narrow therapeutic windows are involved. Careful monitoring for adverse events related to delayed gastric emptying is recommended, particularly in at-risk patients.
Recommendations for mitigating potential issues include:
- Administering azithromycin on an empty stomach may minimize some interactions, though this requires further research to confirm optimal practice.
- Adjusting the dosage or choosing alternative antibiotics when clinically appropriate to lessen the impact on gastric motility.
- Closely observing patients for signs of delayed gastric emptying, including prolonged nausea or vomiting.
Further research is needed to fully elucidate the mechanism and extent of azithromycin’s effects on gastric motility across various populations and dosing regimens. This will allow for more precise clinical guidelines and improved patient care.
Dosage Considerations and Patient-Specific Factors
Azithromycin’s impact on gastric motility is complex and not fully understood, thus precise dosing for this specific purpose lacks definitive guidelines. Always consult prescribing information and a medical professional before administering azithromycin to influence gastric motility.
Renal and Hepatic Impairment
Reduce azithromycin dosage in patients with significant renal or hepatic impairment. Consult relevant guidelines for appropriate dose adjustments based on creatinine clearance or liver function tests. Close monitoring is crucial.
Age and Weight
Dosage adjustments are often necessary for pediatric and geriatric patients. Weight-based dosing is frequently employed in children, while geriatric patients may require lower doses due to potential age-related changes in drug metabolism and clearance.
Concomitant Medications
Certain medications may interact with azithromycin, affecting its metabolism and potentially its impact on gastric motility. Review the patient’s medication history meticulously for potential interactions. Consult a pharmacist or physician if necessary.
Underlying Medical Conditions
Pre-existing conditions, like gastroparesis or inflammatory bowel disease, could influence the response to azithromycin’s potential effects on gastric motility. Tailor the approach accordingly. Individualized patient assessment is key.
Monitoring Response
Regularly assess the patient’s response to treatment, considering both the intended therapeutic effect on gastric motility and potential adverse effects. This helps guide subsequent treatment decisions. Symptoms must be tracked closely.
Disclaimer:
This information is for educational purposes only and does not constitute medical advice. Always consult a healthcare professional for diagnosis and treatment of any medical condition.
Future Research Directions and Unanswered Questions
We need larger, well-designed clinical trials to definitively determine azithromycin’s efficacy in improving gastric motility in specific patient populations. These studies should include diverse demographics and consider comorbidities influencing gastrointestinal function.
Specific subgroups warrant investigation: patients with diabetic gastroparesis, those undergoing chemotherapy-induced nausea and vomiting, and individuals with chronic idiopathic gastroparesis. Each group likely responds differently to azithromycin.
Dosage optimization remains a key area. Studies comparing different azithromycin regimens (single vs. multiple doses, varying total dosages) are required to find the most effective and safe treatment protocol for motility disorders.
Investigating the mechanism of action beyond its macrolide properties is crucial. We need to understand how azithromycin interacts with specific gastric receptors and signaling pathways to improve motility. This knowledge will support the development of more targeted therapies.
Long-term safety and efficacy data are lacking. We need to assess the risk of antibiotic resistance development and the potential for long-term adverse effects from chronic azithromycin use for gastric motility improvement. A thorough assessment of potential drug interactions is also needed.
Biomarker identification holds promise. Identifying reliable biomarkers predicting azithromycin responsiveness could personalize treatment, maximizing benefits and minimizing unnecessary antibiotic use.
Finally, exploring azithromycin’s potential in combination with other prokinetic agents is warranted. Synergistic effects might lead to improved efficacy and reduced dosage requirements for each drug.